SHOULDER REPLACEMENT SURGERY
If your shoulder joint gets seriously damaged, you might need surgery to replace it.
What To Know
If your shoulder joint gets seriously damaged, you might need surgery to replace it. Before you have your procedure, you should know some things.
About Your Shoulder
The joint where your upper arm connects to your body is a ball-and-socket joint. The bone in your upper arm, called the humerus, has a round end that fits into the curved structure on the outside of your shoulder blade.
Ligaments and tendons hold it together. Ligaments connect the bones, while tendons connect muscles to the bone. A layer of tissue called cartilage keeps the bones apart, so they don't rub against each other.
The ball and socket lets you move your arm up and down, back and forward, or in a circle.
Why You'd Need It Replaced
You may have to have it done if you have a condition that makes it painful and hard to use your arm, such as:
• A serious shoulder injury like a broken bone
• Severe arthritis
• A torn rotator cuff
Your doctor will probably try to treat you with drugs or physical therapy first. If those don’t work, they may recommend surgery.
Shoulder replacement surgery is less common than hip or knee replacements. But more than 50,000 shoulder replacements are done in the U.S. each year.
Types of Shoulder Surgery
An orthopedic surgeon will replace the natural bone in the ball and socket of your shoulder joint with a material that could be metal or plastic. It's a major surgery that'll keep you in the hospital for several days. You’ll also need several weeks of physical therapy afterward.
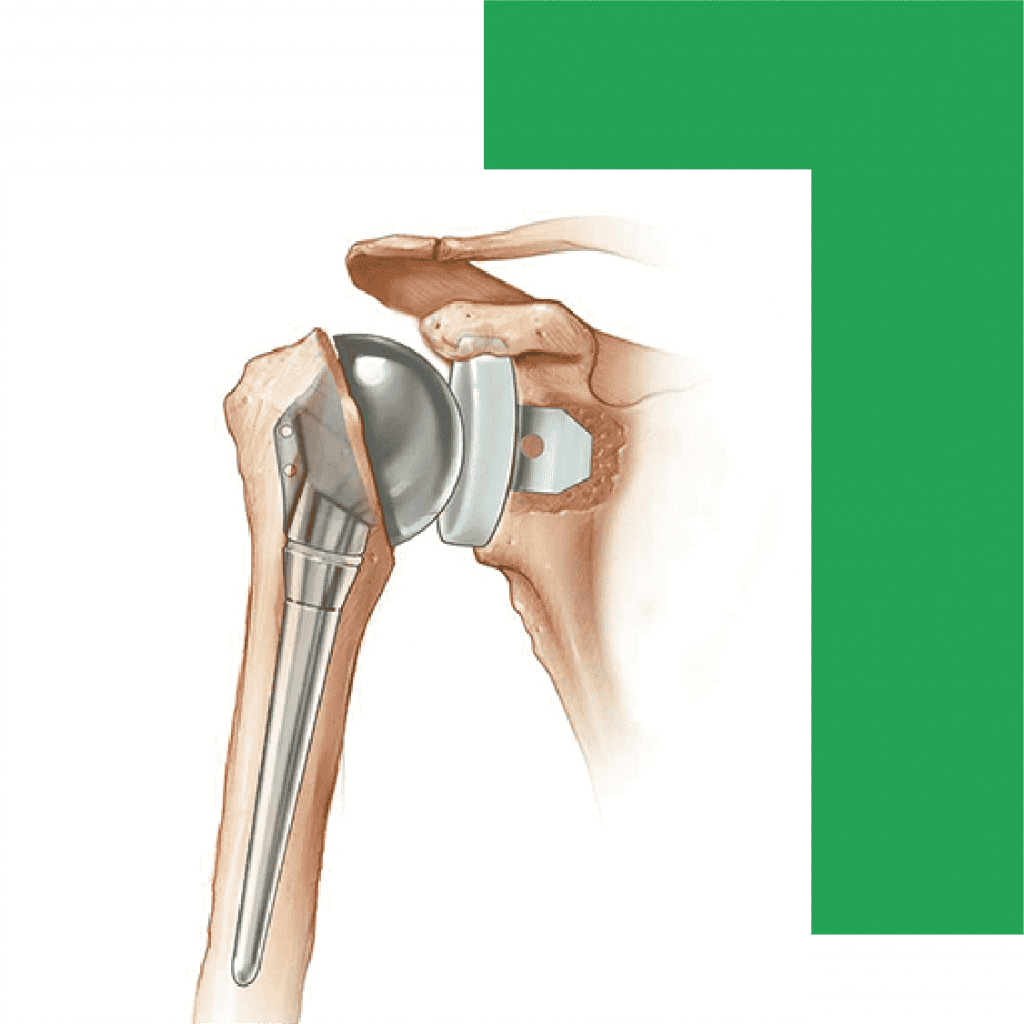
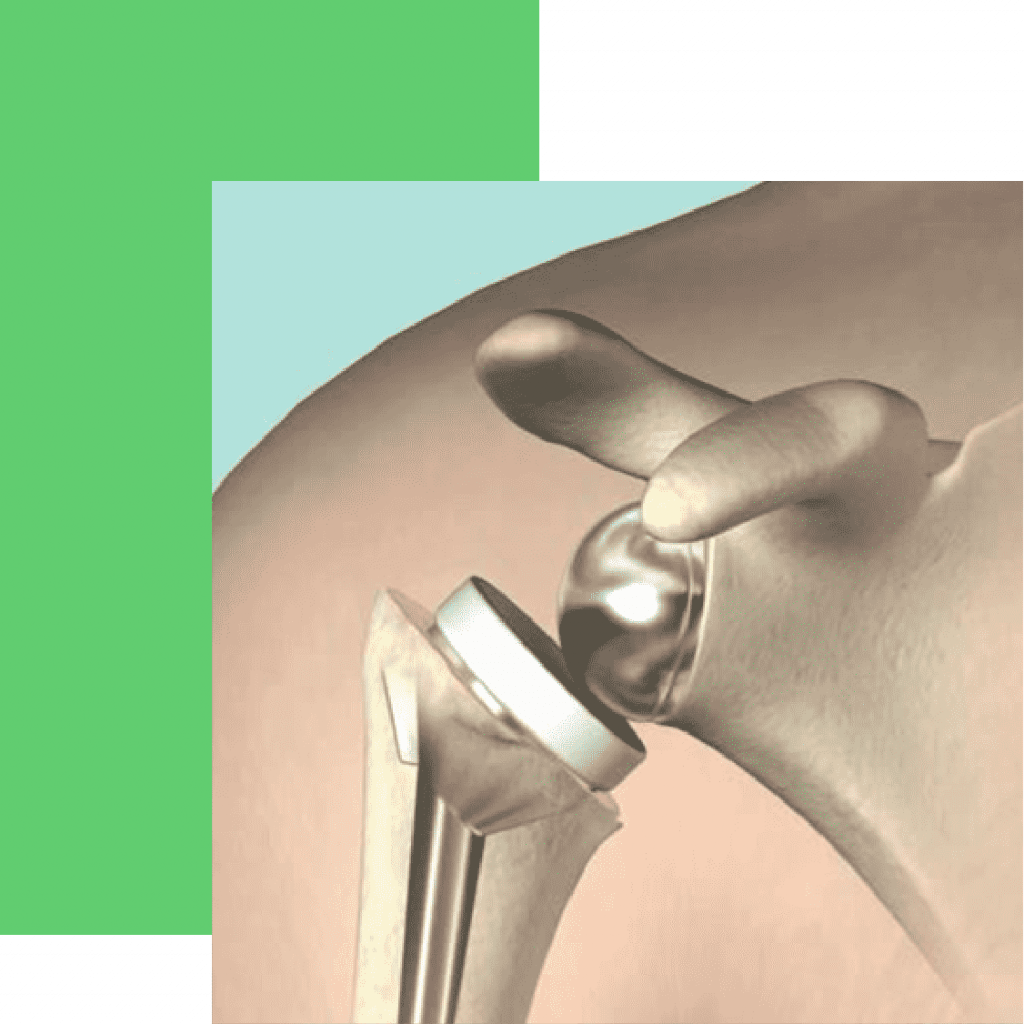
There are three types of shoulder replacement surgeries:
Total shoulder replacement: This is the most common type. It replaces the ball at the top of your humerus with a metal ball, which gets attached to the remaining bone. The socket gets covered with a new plastic surface.
Partial shoulder replacement: Only the ball gets replaced.
Reverse shoulder replacement: Usually, you'd get this if you have a torn rotator cuff. It’s also done when another shoulder replacement surgery didn’t work. The metal ball gets attached to your shoulder bones, and a socket is implanted at the top of your arm.
Preparing for Your Surgery
Before you get your new shoulder, you’ll likely get a full physical exam and X-rays or other imaging tests so the surgeon can get a look at the joint.
Talk to your doctor about any other conditions you have and any medications you take. You’ll have to stop taking certain drugs, especially narcotic painkillers, several weeks before surgery.
You may have to cut back on drinking and get more exercise, too. If you smoke, you’ll be asked to quit. Scientists have found folks who smoke are more likely to have complications from joint replacement surgery than those who don't.
Don’t eat or drink anything after midnight on the night before your surgery.
The procedure takes about 3 hours. Doctors will give you drugs to put you under during the surgery.
You’ll want to be sure you have some help with your daily routine lined up for a few weeks after you come home from the hospital. You won’t be able to move your arm very much. If you don’t have a relative or friend who can help you out, you might want to check into a rehabilitation center until you can do more things on your own.
You may also want to move some things around at home to make them easier to get to while you recover.
RECOVERY
You will likely be able to go home the same day. Your shoulder will swell, and it will hurt. Your doctor will prescribe drugs to help you manage the pain. Cold compresses can help control the swelling.
At first, your arm will be in a brace to keep it from moving. Within a day or so, you’ll start physical therapy to get your arm and your new shoulder working.
You’ll keep doing physical therapy after you go home. You’ll do exercises that will gradually improve how your new joint works. Don’t rush things: It may take 4 weeks before you can pick up anything heavier than a glass of water.
Your arm will be in a sling for most of your recovery. It may be 6 weeks or more before you can drive again.
In the year after your surgery, you’ll have several follow-up visits with your doctor so they can see how your recovery is going.